SPIC — Supportive Peri-Implant Care
Supportive maintenance for healthy peri-implant tissues (primary prevention) and after successful treatment (secondary prevention).
Recall schedule: 3–6 month intervals, tailored to patient risk profile.
Evidence Guidelines & evidence
- EFP S3 R5.4
We recommend peri-implant probing to assess the presence of BOP, and to monitor changes in PD, and changes in the mucosal margin level.
- EFP S3 R5.6
We recommend regular supportive peri-implant care in patients who have healthy peri-implant tissues, to reduce the risk of incident peri-implant diseases, emphasizing to the patient the importance of their adherence to SPIC visits and home care.
- EFP S3 R5.14
The following approaches for dental implant biofilm removal can be used alone or in combination: titanium or stainless-steel area-specific curettes, ultrasonic/sonic instruments, rubber cup or brushes, air-polishing devices with glycine powder or erythritol alone or in combination.
- EFP S3 R8.3
Clinical parameters should be recorded 6 months post-treatment; radiographs obtained at 12 months. Complication-free survival and patient satisfaction should be included in long-term evaluation.
1 Peri-implant probing & assessment
Baseline probing within 3 months of prosthesis delivery. Re-probe at every recall visit (R5.4). BOP assessment at each recall.
2 Patient motivation & OH instruction
Individually tailored oral hygiene instructions at every recall (R5.9). Include interproximal brushes where indicated (R5.15).
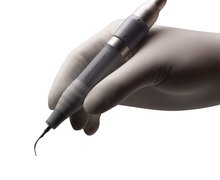
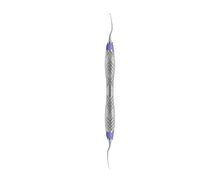
3 Professional mechanical plaque removal
All modalities for dental implant biofilm removal can be used alone or in combination (R5.14): titanium or stainless-steel area-specific curettes, ultrasonic/sonic instruments, rubber cup or brushes, air-polishing devices with glycine powder or erythritol. After treatment (secondary prevention): tailor modality selection to history and tissue response; preserve implant surface over repeated maintenance cycles.
4 Adjunctive healing support (post-treatment)
After successful treatment of mucositis or peri-implantitis, adjunctive measures may be considered to support tissue health and reduce recurrence risk.